Knee Arthritis
Knee arthritis or osteoarthritis is a condition where the ‘hard’ cartilage of the knee is worn or damaged, causing discomfort, an awareness of your knee particularly when walking or weight bearing. It is a very common condition. It can be treated in a number of ways, but before treatment is started, it may be useful for experts to fully assess your symptoms and advise on the many treatment options available to you.
Symptoms Of Knee Arthritis
Pain, discomfort, awareness of your knee when walking, stiffness, tightness, swelling, sudden sharp pain when turning or twisting, a grating feeling when you move the knee may all indicate an on-going problem in the knee, and the commonest cause of this is arthritis or early arthritic changes in the knee, such as a cartilage/meniscal tear, ligamentous rupture/sprain.
The Arthritic Knee
The smooth, slippery hard cartilage that lines the knee gets worn over time and does not regenerate or ‘re-grow’. In essence this loss of hard cartilage is what defines arthritis. This results in pain, stiffness and swelling which with time becomes very debilitating. Eventually hard cartilage is destroyed, allowing the rough bone ends to rub together.
However, before the changes seen above, early arthritis of the knee is often encountered after years of use or overuse and leisure / sports injuries. Patients often complain of an aching discomfort in the front or inside of their knee, aggravated by turning or twisting movements, causing sharp pain or catching/clicking. Walking any significant distance can be uncomfortable, and patients struggle to keep active. In such patients, wear and tear of the meniscus or soft cartilage of the knee is can cause acute pain. Such pain is often aggravated by turning or twisting movements. It is an extremely common problem.
Why Is It Important To Have My Knee Looked At?
If there is one common theme in medicine, it is this: The sooner a diagnosis is made the easier it is to treat the problem. If you are getting symptoms from your knees or are worried it is far better to see a specialist and either have your mind put at rest or the correct diagnosis made and treatment started. This is particularly true for arthritis of the knee (or early arthritis of the knee), more so than any other joint.
The Arthritic Knee
What Happens When I See The Consultant
The first thing you can expect is your consultant to listen to your story about what has been happening – to take a detailed “history” of your symptoms. He will also ask about any history of injury as well as any other health problems you may have.
Mr. Kim will then examine you thoroughly to see exactly what the problem is. At this stage, although your consultant will have a pretty good idea what the problem is with your knee, he will want to arrange further tests to confirm the diagnosis and to make sure there are no other problems which could be the cause. The tests he is likely to consider will include:
Weight Bearing X-Rays
An X-ray of the knee is a simple test/investigation that gives much information about the bones of the knee joint and is often all that is needed to make a diagnosis. Often, dedicated or specialised views of the knee is required to fully appreciate the extent of knee arthritis. (e.g. ‘Rosenberg Views’).
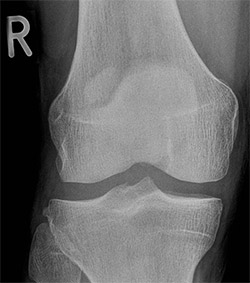 Xray of a normal Knee note gaps between the Thigh and Shin Bone
Xray of a normal Knee note gaps between the Thigh and Shin Bone 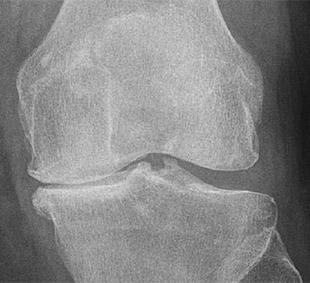 Xray of a Knee with Arthritis note the bone on bone appearance to the left of the Xray typical of Cartilage loss seen in Knee Arthritis
Xray of a Knee with Arthritis note the bone on bone appearance to the left of the Xray typical of Cartilage loss seen in Knee Arthritis
MRI Scan
An MRI (“Magnetic Resonance Imaging”) scan. This is a scan which is particularly useful at showing soft tissues and fluid. It is good for looking at the muscles and ligaments around the knee.
How Is Knee Arthritis Treated?
There are two main ways of treating knee arthritis:
- Non- operative treatment / “Conservative management” – in other words painkillers, knee injections (see below), appropriate exercises and physiotherapy treatment.
- Surgery
Once your consultant has assessed you and taken any X-rays or scans that he feels are necessary, he will discuss with you the best way forward. A great deal will depend upon how bad your symptoms are and how much impact they are having on your quality of life, as well as the underlying cause of the arthritis. For example, there a number of medicines which can be given to treat some of the inflammatory causes of arthritis.
Knee Injections
Knee injections do not cure knee arthritis or cure wear and tear in the knee. However injections may provide improvement in symptoms in patients with mild to moderate knee arthritis i.e. buy time to improve fitness with appropriate exercises (e.g. use of a stationary bike), optimise weight and allow for physiotherapy treatment. These injections are performed in clinic, under strict clean techniques (“aseptic environment”).
There are different knee injection options including:
- Knee Steroid (Cortisone) and local anaesthetic injections. This is an anti-inflammatory injection which can improve symptoms by reducing inflammation associated with early to moderate knee symptoms. These injections can work quickly, but often do not last long. The concerns with repeated injections of cortisone injections are: damage to the hard cartilage and soft tissue, causing further deterioration in the structure of your knee. Please note that if you had a steroid injection which does not work, the minimum interval between this injection and knee replacement surgery (partial or full) is 3 months, due to the risk of deep infection after surgery.
- Hyaluronic Acid injections. These injections aim to improve the viscous and elastic elements of joint fluid, which is affected in patients with knee complaints. Hyaluronic acid is a naturally occurring substance, and unlike steroid injections, may have a cumulative effect in managing symptoms, unlike steroid injections. However, the latest advice does not support the use of these injections in isolation for knee arthritis.
- “Blood Injections” therapy, also known as Platelet Rich Plasma injections (PRP injections). There is evidence that plasma separated and isolated from your own blood may be used in the treatment of knee arthritis. There are different forms of PRP injections, and not all PRP’s are considered the same. For example, recent research would suggest that the higher the number of PRP’s isolated during the preparation of PRP, the better the likely outcomes. Mr Kim will discuss various preparations of PRP with you. There is also evidence that PRP combined with Hyaluronic acid injections may be better than PRP injections on its own. Mr Kim will discuss this with you at your consultation. Although a bit outdated, you will find national guidelines on this via this link: https://www.nice.org.uk/guidance/IPG637/InformationForPublic.
- Arthrosamid Knee injections. Arthrosamid consists of a gel (hydrogel) which is inert (does not react with your tissues) but does not get absorbed. It is designed to become joined up with the lining of the knee, improving cushioning and shock absorption of the knee. This is a novel gel which has been shown to be safe and may be effective in patients with knee arthritis, albeit not in long term studies. It is expensive, is an option if other treatment modalities fail to meet your expectations, and if you do not wish to consider surgical options. Mr Kim and his team would discuss this is detail with you at your consultation and would refer you to patient information sheet/ brochures on this product if you wish. Benefits are improved pain and risks (infection, no effect/ no better in spite of injection, bleeding, temporary effect, non definitive action) should be considered.
- Patients ask about the success of injections, and it is a matter which will be discussed with you, taking into account the severity of your knee arthritis, your particular symptoms and your attitude to risks/ benefits. Generally, if in doubt, please do not proceed with treatment (whether injections or surgery); Mr Kim will take you through each option in a detailed way, and allow you time to reflect on your own individual wishes.
Minimally Invasive Surgery
Knee Arthroscopy/ Keyhole Surgery of the Knee
Keyhole surgery of the knee is not indicated or has no role in treating patients with moderate to severe knee arthritis. The role of key hole surgery of the knee is limited to localised or early osteoarthritis of the knee. Mr Kim and his team will discuss this in detail with you at your consultation.
Surgery For Knee Arthritis
In the end some patients with knee arthritis go on to have surgery for the problem, and one of the big advantages of surgery is the tremendous improvement in quality of life that can result, particularly when it comes to mobility and freedom from pain.
The advances in technology and robotics is such that often partial rather than full joint replacement surgery is now required for patients with severe symptoms. Many people put off surgery for as long as possible, and although this is generally sensible when they finally have their operation, they are so astonished at how much better they feel they wish they had done it sooner!
If we feel the only way to really help with your symptoms is an operation, I will discuss the various surgical options including optimally invasive, partial or personalised knee replacement surgery, exactly what is required from you (in terms of the need for compliance with exercises and rehab after surgery) and go through the details of the surgery recommended. I would often refer you to a physiotherapy colleague if not done already before surgery, to prepare you for surgery and to reassure you that it is the most appropriate option for you.
Knee Replacement Surgery
A knee replacement, or arthroplasty is a surgical procedure in which the damaged or worn portions of the knee are removed and replaced with a new, artificial joint. The operation involves removing the damaged surfaces of the knee and replacing them with an artificial joint containing metal and high-grade polymer. It is a very successful operation for the vast majority of people.
DO YOU NEED A KNEE REPLACEMENT?
You may need a knee replacement if you have difficulties with day to day activities such as walking and climbing stairs. You may not be able to walk or enjoy your leisure activities as much as you wish due to discomfort, an aching awareness of your knee and stiffness and/or swelling.
A knee replacement is a quality of life procedure which should improve these symptoms significantly. Patients who recover after knee replacement often report not just improved physical fitness, improved well-being and but being in better mood.
IS KNEE REPLACEMENT PAINFUL
You will experience pain after a knee replacement, but it is well controlled by a number of ways including the use of regular painkillers and anti-inflammatories and regular icing after several weeks after surgery. You will experience a different type of pain compared to the arthritic pain before surgery, which will improve day by day.
The pain is part of the healing process and due to swelling and inflammation. It may last several months after the procedure, but improves every day. As such, regular icing and anti-inflammatories (if not contra-indicated) and regular stretches as shown by the physiotherapists would help.
When can a partial knee replacement be performed robotically?
POTENTIAL COMPLICATIONS
Although knee replacements are successful operations, there are risks associated with the procedure you must be aware of and accept prior to knee replacement. These risks include infection, clots (‘thrombosis’), pulmonary embolism (where clots go to the lung), stiffness (the commonest complication after knee replacement), pain in spite of surgery (even chronic/unexplained pain/ 1% regret risk), incomplete relief of pain after surgery, general dissatisfaction, nerve and vessel damage, fracture, re-operation, revision risk, medical, anaesthetic and mortality risks (1 in 350 to 1 in 400, according to National Joint Registry). No surgery can be performed without risk, and no surgeon or hospital can guarantee results that would completely meet your expectations. If in doubt, please discuss your concerns with your Surgeon, and delay or not proceed with your operation, as knee replacement is a quality of life procedure, and can be delayed or postponed.
However, you will be reassured we will take every precaution to minimise these risks, including but not limited to, giving you antibiotics before and after surgery, injections or tablets to reduce the risk of clots, medical care, assessment and supervision before and after surgery.
BENEFITS AND RISKS OF KNEE REPLACEMENT SURGERY
THE ANAESTHETIC
You will typically have a regional anaesthetic (spinal anaesthetic), or occasionally for medical reasons a general anaesthetic, and sedation. We will of course, consider your wishes in relation to your preferred anaesthetic. The operation will take between 1 and 2 hours (depending on whether conventional knee replacement or robotic assisted knee replacement or partial knee replacement is performed- read further!).
THE PROCEDURE
A straight cut, usually over the front of your knee is made. The bottom end of your thighbone is trimmed to remove the damaged surface and is then shaped to fit the metal bit of the knee replacement. The damaged top end of your shin bone is removed to make a flat surface. The new parts are fitted over both bones, and tested to make sure they fit and the joint works well.
Once the new parts are fitted and working the wound will be closed using stitches or staples and covered with a large dressing.
RECOVERY FOLLOWING KNEE REPLACEMENT
You will typically be in hospital between 2 to 5 days after surgery. You will need crutches or a walking aid for several weeks after knee replacement. Recovery is a balance between rest and icing the knee to reduce inflammation and swelling, and staying active with increasing walks and exercise. A trained physiotherapist and your Surgeon will guide you through your recovery. In general, listen to your knee. If you do too much, your knee will ache and may swell excessively. If that happens, you must elevate, rest and ice your knee, allowing the inflammation and swelling to subside.
LEADING-EDGE TECHNOLOGY KNEE REPLACEMENTS
Although knee replacements are generally successful in relieving pain and improving function, approximately 15 to 20% patients are not fully satisfied with the procedure, possibly because of increasing expectations of what the procedure should achieve. Increasingly, patients want to forget they had a knee replacement.
WHY ROBOT-ARM ASSISTED KNEE REPLACEMENT?
Robotic-assisted technology has come about as it is appreciated that the precision and accuracy of knee implant placement can be the difference between a ‘good’ and a ‘forgotten’/excellent knee. In robotic assisted knee replacement, your Surgeon could very precisely (to fractions of a millimetre) implant a knee that is tailored to your anatomy, your knee size and alignment. The outcomes following robotic assisted knee replacement are very promising, with patients happy that the technical approach to surgery is extremely accurate, so that they are left with just having to concentrate on the rehabilitation required after knee replacement.
MAKO Robot-arm Assisted Knee replacements and MAKO robot-arm assisted hip replacements
The following are summaries of research supporting the use of MAKO Robot-arm Assisted Knee replacements (total and partial knee replacements) and MAKO robot-arm assisted hip replacements. Over 1 million MAKO robot-arm assisted hip and knee replacements have been implanted worldwide (Stryker Data, March 2023), with its use increasing exponentially. Some insurers are resisting its use due to increased costs involved, but increasing evidence in the literature supports its use, with improved outcomes in terms of quicker recovery, shorted hospital stay, less pain, improved accuracy and precision of the surgical procedure using implants that are tried and tested, with improved outcomes compared to joint replacements implanted manually using conventional methods.
Click here for more information about Mako Total Knee key clinical studies.
Click here for more information about Mako® Partial Knee arthroplasty: clinical summary.
CONSIDERING A KNEE REPLACEMENT? THE NUMBER OF KNEE REPLACEMENTS PERFORMED BY YOUR SURGEON MATTERS.
Research has demonstrated that the number of hip and knee replacement procedures performed (e.g. a year) by treating Surgeons matters, * with better outcomes associated with higher volume hip and knee Surgeons.
Mr Kim performed the largest number of private Robot assisted hip and knee replacements in the United Kingdom with more than 1,500 hip and knee replacements performed
According to the National Joint Registry **, Mr Kim performed :
- 490 total hip replacements (NJR data April 2022 to March 2025)
- 404 total knee and partial knee replacements (NJR data April 2022 to March 2025)
which are significantly higher than the average numbers performed by hip and knee surgeons in the United Kingdom.
Outcomes collected in the National Joint Registry reveal very satisfactory
clinical outcomes in terms of survivorship of the hip and knee replacements and patient safety over the short and long-term.
In addition to the reassuring data available in the National Joint Registry, patient reported outcomes matter. You will find evidence of several patient reported outcomes by clicking on the various links below.
https://www.iwantgreatcare.org/doctors/mr-winston-kim
https://threebestrated.co.uk/orthopaedic-surgeons-in-manchester
TIPS FOR A SUCCESSFUL OUTCOME
Knee replacements are generally very successful operations. However, it is important to be patient, to follow Surgeon and physiotherapy advice/instructions, (e.g. regular icing), to expect that recovery is a process ("good/bad days"), may take 6-9 months to see significant improvement to your symptoms and function. It is important you understand that compliance with physiotherapy and exercises after knee replacement correlates strongly with an excellent outcome. It is also crucial you understand what may or may not be achievable, that is, your expectations must match what the surgeon and physio believe can be achieved in terms of pain relief and improvement in function from having a knee replacement when considering what you were like before surgery.
In short, be patient and rehab well to ensure a good outcome. Mr Kim and his team will ensure that you are seen by trained/specialist physiotherapist and you are fully aware of what is required before and after surgery in terms of patient education, exercises and a fitness and strengthening program of exercises tailored to your needs.
AFTER CARE FOLLOWING KNEE REPLACEMENT
The advantages of having your knee replacement performed privately is that the whole of your care is provided by an experienced Consultant Orthopaedic Surgeon assisted by his team. Your Surgeon will see you daily after your knee replacement, you will have your own room in highly reputable hospitals (BMI the Alexandra or Spire Manchester Hospitals), physiotherapy treatment, medical care if required will readily available including High Dependency or Intensive Care facilities.
Furthermore, you will have ready access to your Surgeon and his team after discharge from hospital (via a phone call, e mail or outpatient visit, as required).
PRICING (GUIDE PRICE- PLEASE CALL FOR FURTHER DETAILS)
-
- Patient pathway
- Initial consultation
- Diagnostic investigations
- Main treatment
- Post discharge care
- Total
-
- Hospital fees
- N/A
- Included
- Included
- Included
-
- Consultants fees
- £285
- N/A
- Included
- Included
-
- Total
- £16,340 to £ 21,765
( robotic assisted surgery, costs dependant on factors such as whether partial knee replacement, preferred implant choice, medical risks such that high dependency/ intensive care needed etc. A breakdown of costs will be confirmed in writing prior to your surgery)
TERMS & CONDITIONS
This is a guide price for your consultation and treatment package. Your consultant will be able to discuss treatment options (e.g. conventional v robotic assisted surgery, and whether ITU care required) and costs with you (subject to your pre-assessment tests) so you are able to make an informed decision that's right for you. The fixed cost will be confirmed in writing at time of booking your treatment. Prices can be subject to change.
WAYS TO PAY
There are three ways to pay for your treatment via BMI Alexandra or Spire Hospital.
- PAY FOR YOURSELF:
Pay for yourself with our fixed price packages. This includes your pre-assessment, treatment, follow-ups and 6 months aftercare - SPREAD THE COST:
Pay for yourself with the finance and spread the cost over 12 months, interest-free (terms and conditions apply) - PRIVATE MEDICAL INSURANCE:
The cost of your treatment may be covered by private medical insurance (check with your insurer first)
Want to find out more? Speak to one of our team today
Post Operative Rehab Guide
Each and every one of us is different and the treatment you will receive is tailored to you, so the most important thing is to follow your surgeons’ advice. After undergoing knee replacement surgery, it is important you have realistic expectations about the types of activities you may perform. Driving, keep-fit activity, walking, and other everyday activities will all be impacted in some way.
Driving
You may return to driving a few weeks after surgery, usually you are given the go ahead once seen at the clinic around the 6-week mark. If the surgery was performed on your right side, we may recommend that you wait longer than if you had surgery on the left side, assuming you drive a car with automatic transmission. In any case you must be able to move the leg easily from the accelerator to the brake, and make a safe emergency stop before driving. That time typically varies from 4 to 8 weeks depending on multiple factors. Always inform your insurance company before going back to driving once given the all clear by your surgeon.
Keep Fit Activity
Your fitness regime will be started in hospital as part of your recovery program. More strenuous activity may be recommended anywhere from 2 to 3 months following surgery. Your surgeon and physiotherapist will discuss different aspects on an individual basis.
Walking And Stairs
You will progress during your physical therapy program from your original walking aid (e.g., walker, crutches) to a cane. If you feel safe stairs are possible from day 1 or 2. You are limited by how safe you feel rather than with the operated knee itself. Eventually no supportive devices will be needed as long as there are no other problems that require long-term use of a walking aid. Eventually you will be allowed to climb stairs step over step. In most cases, patients begin with smaller-height steps and gradually progress to standard-height steps.
Work Activities
Determining the date you return to work will depend both on your surgeon and the type of work you do. Some individuals may require modifications to their job, while others may easily return to their previous activities.
Leisure And Sports
There are different risks associated with certain types of leisure and sport activities. Some activities may lead to damage of your artificial joint over time due to wear and tear of the joint. In general, the more vigorous the activity, the higher the risk of damaging the implant, increasing the wear and tear on the implant, or increasing the risk of loosening or dislocating the implant.
Three major categories of activities should be avoided. These include:
- Activities that cause high-impact stresses on the knee
- Activities with potentially high risk of injury
- Activities that may result in falling or getting tangled with opponents, risking rupture of ligaments around the joint itself or a fracture of the bone around the implant.
These types of activities include competitive racquet sports (such as tennis, squash, and racquetball), high-impact aerobics, high intensity jogging, water skiing, skiing, martial arts, football and basketball. Lower-stress activities such as golf, hiking, walking, cycling and swimming are excellent forms of exercise for individuals with a knee replacement.
The way a knee replacement will perform depends on your age, weight, activity level and other factors. There are potential risks and recovery takes time. If you have conditions that limit rehabilitation, you may require further help prior to having this surgery. Only a specialist knee surgeon can tell you if a replacement is right for you.
Want To Find Out More Speak To One Of Our Team Today
Once you have been assessed (by Surgeon, often Physiotherapist), a treatment plan is discussed with you. You will be given time to reflect on the options available to you.
Frequently Asked Questions:
It is entirely understandable that you will have concerns regarding knee replacement surgery and here I answer some of the most common questions we have been asked over many years of treating patients.
I have pain, stiffness and a grating from my knee but my GP said I was too young/not ready for surgery
Your GP may be right, but arthritis can happen to anyone at any age. The important thing to remember though is that it is important to see an expert, a specialist who has been specifically trained to assess and treat problems like this. The advances in technology, materials and robotics mean instead of a full knee replacement, partial replacements may be indicated. Such surgery is beneficial in preserving most of the joint, saving a joint for total knee replacement when much, much older.
Am I Ready for A Knee Replacement?
Only you and a specialist knee surgeon can decide on when is the right time for knee replacement surgery. Here at Manchester Hip and Knee you can be assured we will discuss the treatment options fully and answer any questions you may have. There is never any rush for elective surgery, and when you are ready to proceed, we will be ready too. Again, advances in technology, materials and robotics may influence the decision to choose more conserving surgery / intervention.
How Old Do I Need To Be For A Knee Replacement?
At the Manchester Hip and Knee Clinic, we tailor each individual patient’s treatment to suit their personal needs, both young and old. This allows more arthritis patients to consider treatments at an earlier age whilst still maintaining an active healthy lifestyle. Knee reconstruction is related to need, not age.
Why Do People Wait So Long To Have Knee Surgery?
Many people delay treatment due to fear, misinformation and a lack of awareness of their options. Often, many of these same people wish they had it done sooner.
What should I Expect When I Decide To Have Knee Reconstruction Surgery?
Your surgeon will explain the procedure to you in the clinic. There will be a pre-operative medical assessment to make sure you are fit and well for the procedure. You will also see a physiotherapist to discuss the “do’s and don’ts” of how to look after your knee replacement and what to expect following surgery.
Will I need to be put to sleep for my knee replacement?
Knee replacement surgery can be performed under general anaesthetic or under spinal anaesthesia, similar to when a woman gives birth. You will be seen by one of our expert anaesthetists during your preparation for surgery and he or she will discuss the options with you and advise the best way forward.
How long does the operation take?
Typically around an hour.
Is the operation painful?
Some discomfort and pain is of course to be expected after any operation and knee replacement is no different. However, the discomfort is usually short-term and I always give my patients pain relief to take regularly during whilst they are recovering from surgery. The key is to understand the importance of
- Regular icing of the knee (e.g. 20 min every hour for 6 to 8 times a day, for at least the 1st 4 weeks if no more)
- Regular painkillers (ideally anti-inflammatories, but you must check with us, in case of contra-indications or allergies)
- Elevation at rest (a low stool should suffice)
- Stretches focused on regaining your knee bend (use opposite leg to hook your operated knee backwards when you’re sat down)
- Walk short distances, little and often, with your walking aid, taking care not to overdo things, as it would swell up your knee excessively.
How many nights will I need to stay in hospital?
This depends upon the type of procedure you have as well as your own general health. Generally, patients stay in hospital for 1 to 3 nights and we always try and get people home as soon as they are ready to leave, comfortable and able to cope at home. We work very closely with our physiotherapists to make sure you only leave hospital when you are ready and medically fit to be discharged home safely.
How long will I need to be off work?
This varies depending on your occupation. For desk-based jobs, it is possible to perform some work from home between 3-4 weeks after surgery. The ideal situation is to take off 6-8 weeks (up to 3 months off work) to minimise swelling and maximise rehabilitation time with the physiotherapists, and do time to do the stretches and icing recommended above
How Long Will Recovery and Rehab take?
After surgery, a few days in hospital are normal. Although we try to get patients home as soon as they are ready and able there is no rush at all. Like your surgery, we tailor your post-op recovery according to your needs. It would typically take 6-9 months (possibly up to 12 months) before you begin to feel really satisfied with the knee. The time to full recovery is often correlated with how you, as the patient, works at your rehab and exercises. Research suggests that you are better at 6 months versus 6 weeks, and even better at 2 years than 1 year post op, and at 5 years, you are better than at 2 years post op, in general.
This is because muscular strength takes time to improve, scar tissue needs time to mature, muscle tightness (invariably present immediately after surgery) needs to improve as well as your confidence and balance. Please always bear in mind that recovery is not a linear upward graph, but full of ups and downs, a journey of recovery. The reward is significantly improved function and symptoms (not guaranteed though) in the majority of patients. Mr Kim and his team is more than happy to navigate this journey with you. They say: (I’m paraphrasing) a journey of a thousand miles begins with the first step…
Patient Testimonials / Recommendations / Reviews by Patients Treated by Mr Kim and Team:
Bernard Sumner, founding member of 2 of the greatest Bands ever (New Order and Joy Division), after successful robot assisted minimally invasive knee surgery, sent 2 overflowing boxes of signed CD’s, vinyl, memorabilia shared by all the team. Surgery by Mr Winston Kim and staff.
Written by a retired General Practitioner
I suffered from Osteoarthritis for a year and was in great pain. I saw Mr Kim in February this year privately. He operated on me and did a Total Knee Replacement in March. i had very little pain post operatively and was discharged in 3 days. I have excellent straight leg raising and a good angle on my knee, up to 120 degrees. I drove after 6 weeks and i have just come back from a holiday in Portugal. A general practitioner friend recommended Mr Kim to me for which i am very grateful. I highly recommend Mr Kim to any patient with knee joint problems.
Dr Enid Noronha, Retired General Practitioner Worsley and Boothstown
Written by a carer
The “Go To” Hip & Knee Surgeon…… Winston Kim, to me, is the “go to” Hip and Knee Surgeon in Greater Manchester. I’m a health care professional and have seen him at work. This is a gifted surgeon- the full package- talented, well trained, generous with his time, humble (if that is possible in a surgeon) and above all, a caring Surgeon. I chose to ask Mr Kim to care for uncle Jim at the Alexandra Hospital. I have seen him look after some really tough cases, and many retired doctors and consultants have placed their trust in him, and had him operate on them. My 90 year old uncle had severe longstanding knee pain, but had refused surgery for ages putting up with pain. Mr. Kim picked up the fact that it was referred pain from the hip, even though my uncle had no hip pain. His confidence reassured us. He did a hip replacement, and gave Uncle Jim a new lease of life. “You put your life and your trust in your surgeon’s hands. Mr. Kim has given me back my life and rebuilt my trust….”, reads one of over 100 reviews online on him- check it out for yourself!. (www.iwantgreatcare.org). But, I knew that already….. P Ryder, Manchester, on behalf of Uncle Jim, April 2015
Written by a patient
Mr Kim performed my total knee replacement last September which is a complete success. I have been delighted with all the care and consideration he has shown me. He has installed me with a great deal of confidence and I believe him to be a fine surgeon who I would highly recommend. Yvonne Field
Written by a patient
I found Mr Kim most informative about the injury to my knee. He fully explained the extent of my injury and also explained in clear terms the treatment I was to have and the recuperation period and exercises needed for a full recovery. Most impressed with his calm and informative manner and allowed me to ask questions about my injury which enabled me, through his concise responses, to better understand the limits that would be placed upon my future exercise regimes. It helped that the physiotherapist I attend had knowledge of Mr Kim, through other patients, and her confidence in him supported my own views fully supported those on myself. An excellent physician who made an excellent job of my injured knee that has resulted in me returning to by normal exercises with no restrictions or negative after effects. I have recommended him to friends and colleagues and I can think of no greater compliment I can add to the above comments. My name is Arthur Edward Roberts dob 10.12.44., and had my operation on the 17.11.2014.
Written by a patient
I had a full left knee replacement in March 2014. Mr Kim was a most excellent consultant both before and after the operation. His manner was most encouraging and helped me cope with the unknown journey of recovery. Of course Mr Kim did the technical job and was supported by an excellent operating team. The hospital staff and as an outpatient for physio were all excellent in aiding my recovery. I now have almost 100 per cent recovery after 12 months. I am far better off then when I started on this road, I would recommend Mr Kim to anyone. He is a most charming person and has a wonderful manner, just what you want.
Written by a patient
Mr Kim performed my knee arthroscopy in December 2014 at BMI-The-Alexandra-Hospital and I was very impressed with my physical fitness, movement and pain free knee after the procedure. At my six weeks post op appointment, Mr Kim explained in detail what he had done, giving me advice on future exercising -ie- what to avoid etc. His excellent approach with his patients, made me feel at ease and confident about future scenarios with my knee. The physio that was put in place couldn’t have been better and this also contributed my speedy recovery. I completely trust Mr Kim’s experience, knowledge and expertise of orthopaedic surgery and would recommend him.
Listen to a testimonial from a young patient who had a partial knee replacement
REFERENCES
- Malik AT, Jain N, Scharschmidt TJ, Li M, Glassman AH, Khan SN. Does Surgeon Volume Affect Outcomes Following Primary Total Hip Arthroplasty? A Systematic Review. J Arthroplasty. 2018 Oct;33(10):3329-3342. doi: 10.1016/j.arth.2018.05.040. Epub 2018 May 31. PMID: 29921502.
- Kugler CM, Goossen K, Rombey T, De Santis KK, Mathes T, Breuing J, Hess S, Burchard R, Pieper D. Hospital volume-outcome relationship in total knee arthroplasty: a systematic review and dose-response meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2022 Aug;30(8):2862-2877. doi: 10.1007/s00167-021-06692-8. Epub 2021 Sep 8. PMID: 34494124; PMCID: PMC9309153. – NJR data from April 2019 to March 2022
You will need the Adobe Reader to view and print these documents.